Friday, December 23, 2005
Appendicitis and The CT scanner.....
A commenter to this post by the Grunt Doc has resurrected the debate over the appropriateness of CT scanning to look for appendicitis. I will repost the well-written comment:
One issue I have with this study is that the most recent data is about six years old, while the data from the above studies is much more recent. CT scanning has improved much over the past six years and the techniques for performing and interpreting these studies has improved as well. Another is that from the data, the more CT/US that was done, the rate of NA fell. Looking at the following figures:
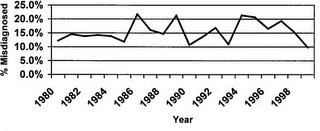 This represents a running percentage of NA during the study period.
This represents a running percentage of NA during the study period.
 This represents the percentage of patients who underwent CT/US during the study period. As you can see the peak usage of CT/US correlates with reduction in the rate of NA.
This represents the percentage of patients who underwent CT/US during the study period. As you can see the peak usage of CT/US correlates with reduction in the rate of NA.
And at least in my institution more than 40 percent of patients with RLQ pain are having CT/US done. Another question not answered, how many patients with "equivocal" exams were sat on and then ruptured in this study? While there is much debate on NA after CT there is little evidence that CT is missing appendicitis.
This debate will rage on, at least until studies utilizing 16 and 64 slice scanners begin to come out. For now we will have plenty to argue about. |
A commenter to this post by the Grunt Doc has resurrected the debate over the appropriateness of CT scanning to look for appendicitis. I will repost the well-written comment:
My wife, a fellow emergency physician here at Landstuhl Regional Medical Center (Germany), had a 30yo male with classic signs for appendicitis (i.e. RLQ pain, RLQ ttp, rebound, guarding) a few nights ago. After completing her Hx and PE she called the SOD (surgeon of the day) for a consult stating that she believed her patient had an acute appendicitis that required surgical intervention. The surgeon, of course, asked her what the CBC and UA results were... She stated that they were still pending.The subject of missed diagnosis lawsuits has been raised by guest-blogger Dr. Tony at Kevin MD as well as his own site. I have not heard of lawsuits arising from removing a normal appendix, but I have seen cases referred for peer review in my hospital. The patients were much like the one described above, young males with a classic presentation. At my institution the default setting seems to be to get a CT scan first and call later. If the CT is negative the patient is discharged or admitted to their PCP's for further evaluation. So not only can unnecessary operations be avoided, hospital stays for "serial exams" can be as well. The lay press is on the case as well:
The SOD went off on her questioning her reasoning for a surgical consult without the benefit of laboratory results... Taking the high road she calmly stated that the labs were pending and would be resulted shortly after his arrival to the ED. Upon his arrival he berated her in front of the entire ED staff for a premature consult. Again, taking the high road, she thanked him for arriving in the ED so quickly and directed him to the patient's bedside. Moments after examining the patient he filled out a buck slip and took the patient to the OR for his appendectomy -- the labs were still pending as he wheeled the patient to the OR...
During his tirade, the SOD told my wife that he would be interested to hear what her colleagues' positions are on calling for a surgical consult prior to labs being resulted -- keep in mind that this patient was a "classic" presentation of acute appendicitis. My response was as follows (not all references used in this informal e-mail are listed -- it was never intended for publication so please forgive any plagiarism of Tintinalli):
Per our discussion....
I believe patients with abdominal pain can be broken down into four groups:
1. Patients who demonstrate classic presentation for acute appendicitis
2. Patients with signs and symptoms that are suspicious but not diagnostic for appendicitis
3. Patients with abdominal pain in whom appendicitis is considered to be a remote diagnostic possibility
4. All high-risk special populations presenting with abdominal pain (i.e. elderly, pediatric, pregnant, immunocompromised)
When evaluating a patient in group one I believe immediate surgical consultation is appropriate... While I would draw the usual labs (i.e. CBC, UA), I would NOT wait for their results before consulting surgery. After all, surgery is going to see this patient whether their WBC count is 8 or 80. Why delay surgical evaluation when the CBC and UA results will not change your decision to have this patient evaluated by a surgeon? The patient you described to me clearly fell into group one. I believe the surgeon would agree seeing as how he took the patient straight to the OR and removed his appendix. The finding of a normal appendix during surgery, while indicative of a misdiagnosis, should NOT be considered an error in the patient's care. After all, a certain percentage of normal appendices should be removed by every general surgeon during the routine performance of their duties - cast a broad net and all... And while the historical accepted incidence of removing a normal appendix 20% of the time is no longer the gold standard due to the advances made in CT and US (Townsend: Sabiston Textbook of Surgery, 17th ed., Copyright © 2004 Saunders, An Imprint of Elsevier. P 1387), the occasional removal of a normal appendix when dealing with patients in group one is to be expected.
As for the CBC - "The WBC is of limited value. The sensitivity of an elevated WBC above 10,000/uL in acute appendicitis is 70 to 90 percent, but the specificity is very low. More important, the positive and negative predictive values of an elevated WBC in acute appendicitis are 92 and 50 percent, respectively (Vermeulen B, Morabia A, Unger PF: Influence of white cell count on surgical decision making in patients with abdominal pain in the right lower quadrant. Eur J Surg 161:483, 1995. Hoffman J, Rausmussen O: Aids in the diagnosis of acute appendicitis. Br J Surg 76:774, 1989. Marchand A, Van Lente F, Galen RS: The assessment of laboratory tests in the diagnosis of acute appendicitis. Am J Clin Pathol 80:369, 1983.)."
As for the UA "Abnormal urinalysis results, excluding proteinuria, are found in 19 to 40 percent of patients with acute appendicitis. Abnormalities include pyuria, hematuria, and bacteriuria, possibly related to the extension of appendiceal inflammation to the ureter (Kretchmar LH, McDonald DF: The urine sediment in acute appendicitis. Arch Surg 87:209, 1963. Puskar D, Bedalov G, Fridrih S, et al: Urinalysis, ultrasound analysis, and renal dynamic scintigraphy in acute appendicitis. Urology 45:108, 1995.)."
In conclusion, I agree with the immediate surgical consultation when caring for a patient that falls into group one. That is how I was trained. That is how I currently practice. That is how I will continue to practice. If the surgeon chooses to delay their evaluation until the labs are resulted then I must concede that making that decision falls within the scope of their practice. And they, of course, will then be held responsible should their decision to delay evaluation results in a poor outcome for the patient - albeit unlikely... Bottom line, however, is that an immediate surgical consult is clearly indicated in group one patients. The decision to wait for lab results and/or imaging and the ultimate decision of cut versus do not cut falls within the bailiwick of the surgeon being consulted on the case. I would have called before the labs were resulted...
END OF E-MAIL TO MY WIFE
As you may have deduced -- the patient did NOT have an acute appendicitis. I think he turned out to have a kidney stone!!!
I would be interested to hear the perspectives of other EP's out there regarding when to call for a surgical consult on patients that fit into group one (listed above)...
But recent research has questioned that tolerance of error, showing that unnecessary appendectomies are both risky and expensive. A University of Washington study found that, among adults, unnecessary appendectomies typically resulted in a six-day hospital stay, while one patient in 40 develops serious complications and 1.5 percent of the patients die.Doing a PubMed search for "appendicitis ct" gave, as expected, plenty of results. Here are just a few:Rapid CT diagnosis of acute appendicitis with IV contrast material.
Dr. David R. Flum, an assistant professor of surgery at the University of Washington in Seattle who led the 2002 study, estimates that Americans paid $741.5 million for unnecessary appendectomies on adults in 1997, the year on which his study focused.
The purpose of this study was to determine the sensitivity and specificity of computed tomography (CT) without administration of oral contrast in confirming suspected acute appendicitis. One hundred seventy-three patient studies were retrieved by a computer-generated search for the word "appendicitis" in radiology reports. Patients presenting to the emergency department over an 8-month period were examined for acute abdominal pain or suspected acute appendicitis. IV-contrast-enhanced CT scans of the abdomen and pelvis were obtained without oral or rectal contrast. Criteria for diagnosis of acute appendicitis included a dilated appendix (>6 mm), periappendiceal inflammation, or abscess. Final diagnoses were established with surgical/clinical follow-up, histopathological analysis or both. The standard time (1 h) for the administration of oral contrast prior to the CT scan was eliminated. Fifty-nine CT diagnoses were made of acute appendicitis, 56 of which were histologically verified and three of which resulted in another diagnosis. One hundred fourteen CT diagnoses were negative for appendicitis. This corresponds to a sensitivity of 100% and specificity of 97%, a positive predictive value of 95%, and a negative predictive value of 100%. CT with IV contrast is sensitive and specific for the confirmation or exclusion of acute appendicitis. By eliminating the time required to administer oral contrast, the diagnosis might be made more rapidly.and:Clinical guidelines, computed tomography scan, and negative appendectomies: a case series.
INTRODUCTION: Prior studies suggest that preoperative abdominal computed tomography (CT) scan can contribute to a low negative appendectomy rate. Our study objective was to evaluate cases of negative appendectomies for clinical criteria and CT use. METHODS: Retrospective 1-year study of all negative appendectomies at a community hospital. Data included clinical evidence for appendicitis as well as CT results if performed. RESULTS: Of 122 cases reviewed, 8 (6.6%) were negative appendectomies. Six were younger than 20 years. Four had a preoperative CT scan. Overall, 106 (87%) of 122 cases received preoperative CT and had a negative appendectomy rate of 3.8%. Sixteen cases did not have preoperative CT and had a negative appendectomy rate of 25% (odds ratio, 8.5; 95% confidence interval, 1.9-38.5; Fisher exact test P = .01). CONCLUSION: Patients who had a CT scan for suspected appendicitis had a lower rate of negative appendectomies than those who had no CT. Most of the negative appendectomies occurred in patients younger than 20 years.A overall negative appendectomy (NA) rate of 6.6 percent is lower than the "historically acceptable" rate of NA which is about 15 percent. The contrast between NA rates between those who received a CT and those who did not was pretty impressive. One needs to remember that the 15 percent historical rate is based on all comers. The rate will be lower in patients such as the one described above, and higher in other groups (women, extremes of age), perhaps even as low as the rates mentioned in the above studies. As a caveat I will mention that I do not have full access to the above articles. If someone else does and wishes to take issue with me, please be my guest. A third study, for which I have reviewed the entire text, is :Misdiagnosis of appendicitis and the use of diagnostic imaging.
Background
CT and ultrasound (US) are increasingly recommended to establish the diagnosis of appendicitis, but population-based rates of misdiagnosis (negative appendectomy [NA]) have not improved over time. The objective of this study was to determine the relationship between CT/US and NA in common practice.
Study design
Using data from the Group Health Cooperative on all patients undergoing appendectomy between 1980 and 1999, a longitudinal study was conducted to determine the frequency of NA over time and a case-control, medical recordÂbased study of a subset of patients from the 1990s was conducted to determine the accuracy of CT/US.
Results
Of 4,058 patients undergoing appendectomy (mean age 31 ± 18.6 [SD] years, 49.6% women), 631 (15.5%) had an NA. The overall incidence of NA remained stable over time at 1.5/10,000 patient-years, as did the age and gender adjusted rate (incident rate ratio 0.95, 95% CI 0.97, 1.01). In 1999, nearly 40% of patients had either CT or US. The aggregate sensitivity of these tests was only 74.2% (95% CI 65.7, 83.7), with a positive predictive value of 95.1% (95% CI 91.5, 96.8). CT scans were 88.3% sensitive, with 97.2% positive predictive value (95% CI 92.9, 100). Ultrasounds were 69.5% sensitive, with a positive predictive value of 94.1% (95% CI 89.6, 96.4). More than one in five tests obtained in patients with NA were positive for appendicitis (21.7% for CT and 20.8% for US).
Conclusions
The rate of NA was unchanged over time despite the introduction and use of CT/US, and this appeared to be related to the inconsistent performance characteristics of the tests. This study cautions against overreliance on CT/US in diagnosing appendicitis and emphasizes the need for test benchmarking in routine practice before establishing protocols for presumed appendicitis.
One issue I have with this study is that the most recent data is about six years old, while the data from the above studies is much more recent. CT scanning has improved much over the past six years and the techniques for performing and interpreting these studies has improved as well. Another is that from the data, the more CT/US that was done, the rate of NA fell. Looking at the following figures:
 This represents a running percentage of NA during the study period.
This represents a running percentage of NA during the study period. This represents the percentage of patients who underwent CT/US during the study period. As you can see the peak usage of CT/US correlates with reduction in the rate of NA.
This represents the percentage of patients who underwent CT/US during the study period. As you can see the peak usage of CT/US correlates with reduction in the rate of NA. And at least in my institution more than 40 percent of patients with RLQ pain are having CT/US done. Another question not answered, how many patients with "equivocal" exams were sat on and then ruptured in this study? While there is much debate on NA after CT there is little evidence that CT is missing appendicitis.
This debate will rage on, at least until studies utilizing 16 and 64 slice scanners begin to come out. For now we will have plenty to argue about. |






